Royal Wound Care is the nation’s leading provider of advanced wound care.
Royal Wound Care is a dedicated wound care center located in West Hills, California, specializing in advanced, comprehensive wound treatment. Founded by Dr. Moaddel, Royal Wound Care was born from his commitment to improve the way patients experience wound care. After witnessing the need for more compassionate, personalized care, Dr. Moaddel opened his own center to ensure that every patient receives the attention and expertise they deserve.
After witnessing the shortcomings in traditional wound care settings, Dr. Moaddel set out to create a better experience—one where patients receive the focused, attentive care they truly deserve. That vision became Royal Wound Care.

Our Mission
To deliver exceptional, accessible wound care tailored to the individual—whether in our state of-the-art clinic, at a skilled nursing facility, or in the comfort of a patient’s home. We treat the wound, but we also care for the whole person.
Why Choose Royal Wound Care?
Ongoing Education & Certification
For staff, families, and partner facilities, including wound in-services and professional training opportunities

Expert-Led Care by Board-Certified Providers
With years of hands-on experience managing chronic and complex wounds

Advanced Modalities
Including negative pressure therapy, mist ultrasound, debridement, Doppler studies, grafts, and more

Survey-Ready Documentation
That keeps facilities compliant and families informed
Truly Personalized Care Plans
Tailored to each patient’s condition, lifestyle, and healing goals

Mobile Services That Come to You
Care delivered at home, in clinics, or within partner facilities

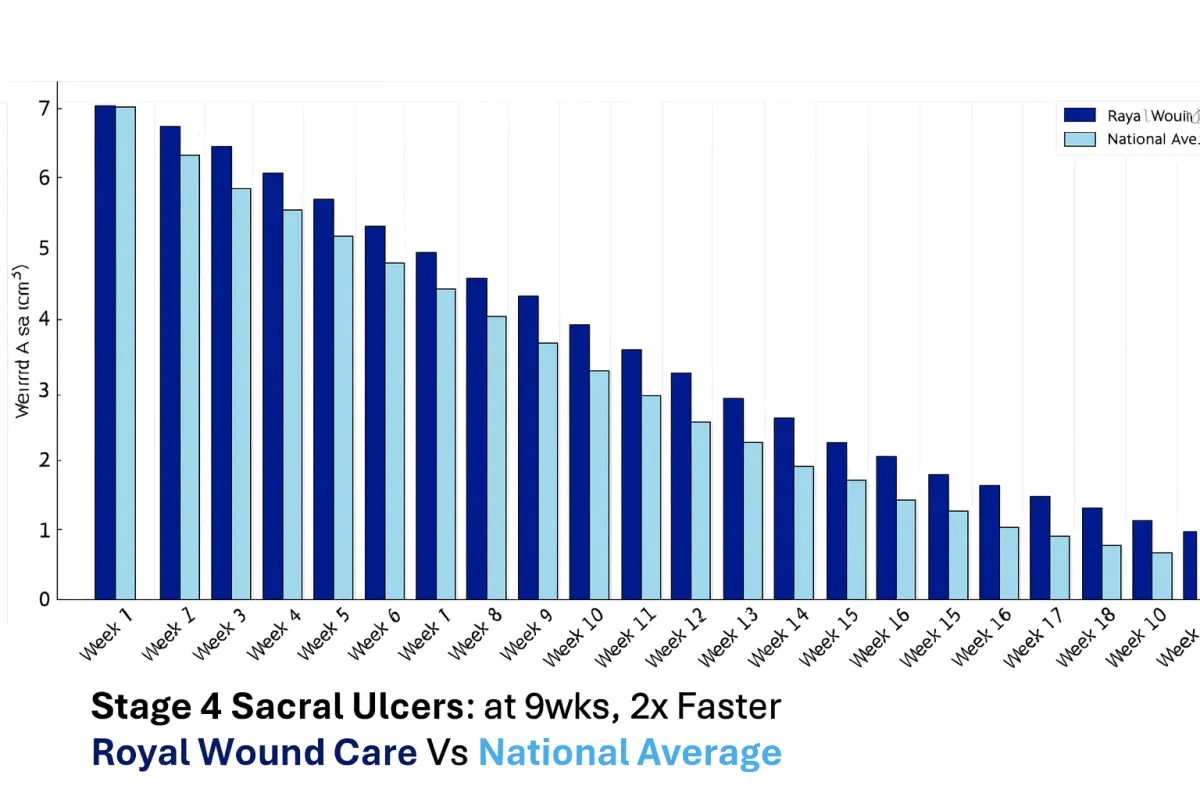
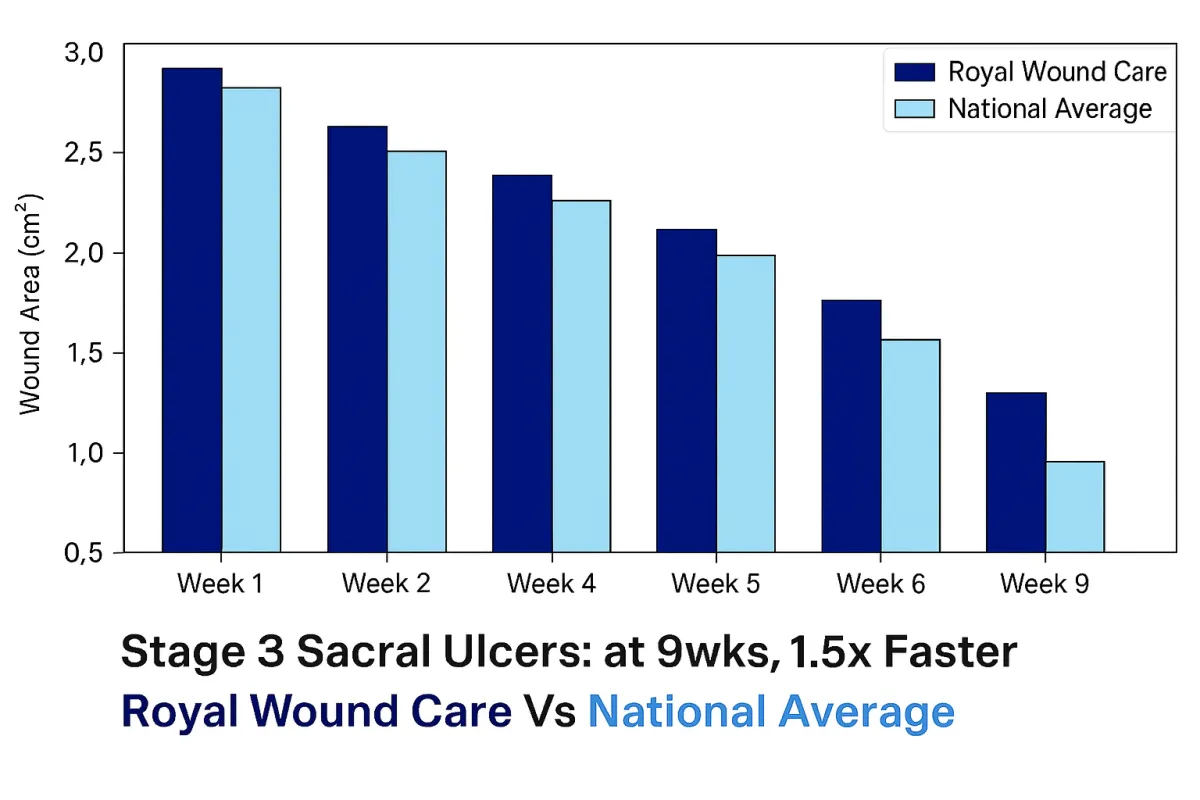
A Team That Cares And The Results To Prove It
At Royal Wound Care, we deliver results that consistently outperform the national average. Our advanced healing process combines evidence-based treatments, personalized care plans, and direct physician oversight to ensure optimal outcomes. Unlike many clinics, every patient is managed by a board-certified wound care physician who evaluates their condition and customizes treatment from day one.
Our Stage 3 Sacral ulcer graph demonstrates how our approach leads to significantly faster healing compared to the national average. While traditional care results in gradual wound size reduction over several months, patients treated at Royal Wound Care experience more rapid progress through targeted therapies, aggressive infection control, and ongoing physician-directed adjustments to their care plan. Our proactive methods allow us to close even complex wounds weeks earlier than national trends, improving patient mobility, reducing pain, and preventing further complications.
Stage 4 sacral ulcers are among the most complex wounds to treat, yet our outcomes set us apart. Patients at Royal Wound Care heal twice as fast as the national average by leveraging advanced biologic grafts, comprehensive infection management, and customized care protocols. These results highlight our proactive, physician-led care model, allowing us to manage even the most challenging cases successfully while improving long-term patient outcomes.
What Our Partners Experience
86% lower infection rates
47% faster healing compared to others
88% fewer wound-related rehospitalizations
58% faster pressure ulcer healing times

Ready to Heal with Royal Wound Care?
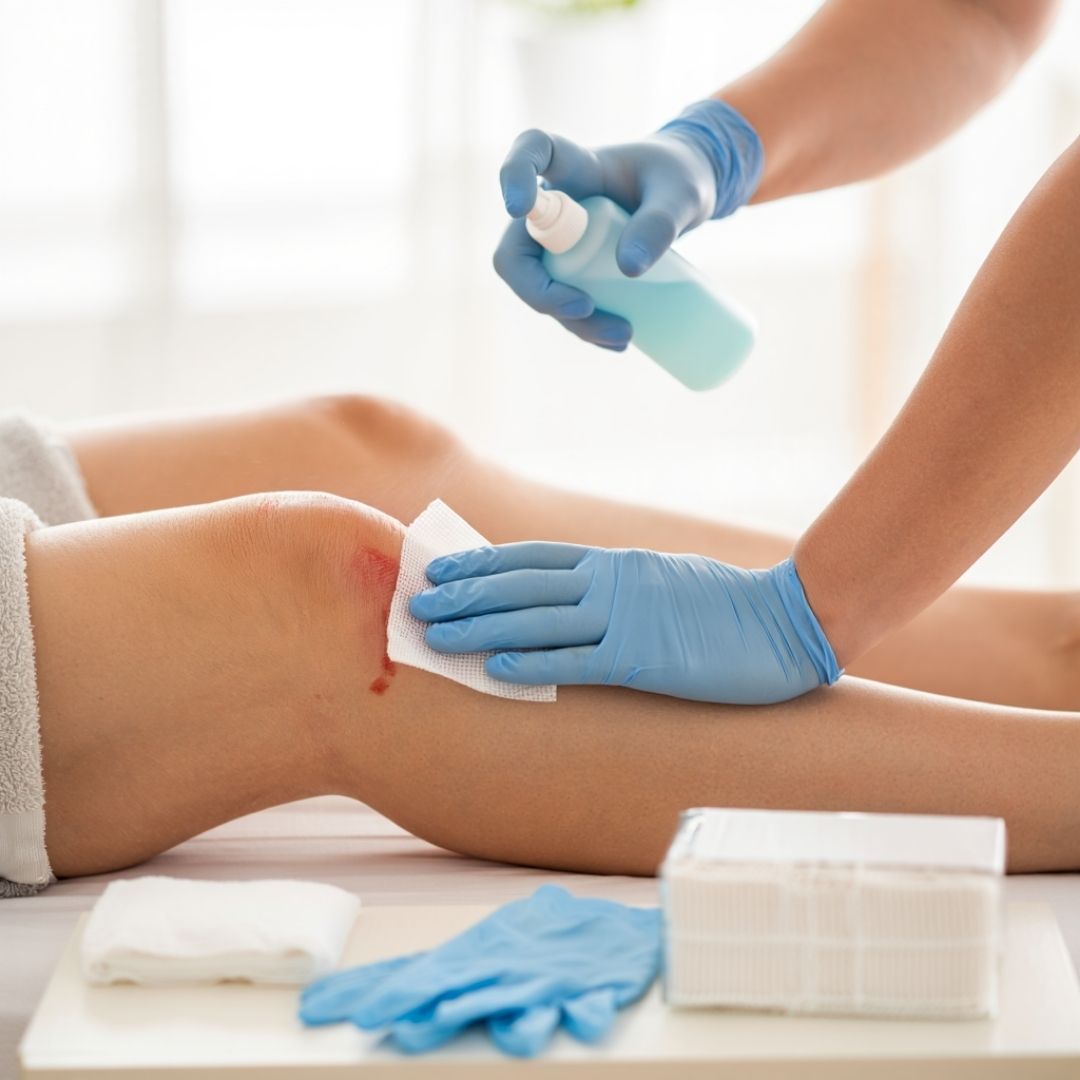
How to Remove Gauze Stuck to Wound Without Pain: Step-by-Step
How to Remove Gauze Stuck to Wound Without Pain: Step-by-Step
From minor lacerations to more severe diabetic foot ulcers, various types of wounds make up the field of wound care. For many patients, gauze often plays an essential role in both proper care and optimal recovery. However, it’s not uncommon for gauze to stick to the wound bed, making removal painful—or even harmful.
This common dressing plays a key role in absorbing drainage, protecting the wound from bacteria, and helping maintain a moist environment to support new tissue growth. However, when it’s adhered to the wound bed, it can increase the risk of infection and potentially hinder healing. Fortunately, it is possible to safely and effectively remove gauze stuck to a wound.
In this guide, we’ll discuss how to properly remove gauze stuck to a wound without pain—while protecting new tissue and supporting proper healing. We’ll also cover why gauze sticks to wounds in the first place and what happens if it’s left too long. This information is essential to preventing wound dressing adherence in the future.

How to Remove Gauze Stuck to Wound Without Pain: Step-by-Step
If you’re dealing with gauze sticking to a wound, know that you’re not alone. It’s an extremely common experience. However, that doesn’t mean it isn’t painful for the patient or that it isn’t aggravating to the healing process. Luckily, this isn’t a permanent problem, and removal isn’t as complex as most think.
At Royal Wound Care, we believe that recovery should be accessible to all—which is why this guide is designed to be informative, easy to follow, and reassuring. We’ll explain why gauze sticks to wounds and provide step-by-step instructions for safe removal. We’ll also cover when to seek medical care and how to support wounds as they heal.
Related: When to See a Wound Care Specialist: Signs It’s Time to Get Expert Help

Why Does Gauze Stick to Wounds?
Gauze sticks to wounds when it absorbs fluid, dries out, and adheres to both damaged and healthy skin.
As wounds heal, they naturally release a mixture of fluids and cells known as wound exudate. This is an essential part of healing as it provides a moist environment, promotes cell migration, and delivers nutrients to the cell bed.
However, it’s also what causes gauze to become stuck to the skin—even with frequent dressing changes. Several factors can increase the likelihood of gauze sticking, including:
Open wounds that drain too much can overly saturate gauze
Wet-to-dry techniques that harden to the skin and make removal complex
Longer intervals between wound dressing changes
Lack of non-adherent dressings
Letting the wound and the gauze dry out completely
Additionally, certain wounds are more prone to dressing adherence, such as venous leg ulcers, burns, and diabetic wounds. Ultimately, this is why caregivers, nurses, and individuals treating a wound should use high-quality, properly selected dressings. For a comprehensive breakdown of different dressing types, visit our guide, “Wound Dressing for Pressure Ulcers.”
Related: How to Treat Venous Ulcers and How Can a Diabetic Wound Heal Faster?
Can You Leave Gauze Stuck to a Wound?
Many patients prefer to leave gauze stuck to a wound to avoid the pain of removing it and the fear of damaging healing tissues. However, we highly recommend removing it as soon as you realize it is stuck. If a gauze is left stuck to a wound, it slows healing, increases infection risk, and can lead to life-threatening complications—such as sepsis or abscesses.
More specifically, leaving gauze stuck to a wound can:
Result in loose cotton fibers getting left behind, which act as foreign bodies that increase the risk of infection
Prevent the blood clot from forming and disrupting recovery
Disrupt the moisture balance and dry the wound bed out
Trap bacteria and debris, leading to potential abscess formation, inflammation, or chronic wound
Most importantly, if the gauze is stuck, do not rip or remove it as quickly as possible. Doing so can cause trauma to the injury and remove fragile healing tissue, damaging the wound and slowing recovery.
Instead, below is a step-by-step guide for safely removing gauze stuck to a wound. We are basing this information on ongoing education, expert-led research, and evidence-based treatments.
Related: How Long Does It Take for a Wound to Heal? What Every Nurse and Patient Should Know

How Do You Remove Gauze Stuck to a Wound?
Step 1: Wash Your Hands Thoroughly
Before touching or removing the dressing, it’s crucial to thoroughly wash and dry your hands. Unwashed hands carry many invisible germs and bacteria that can unknowingly transfer to the injury.
Therefore, if that bacteria enters the wound, it can increase the risk of infection and compromise the new, delicate tissue. To be extra cautious, wear latex gloves after washing your hands.
Step 2: Soak the Gauze to Loosen It
It’s important that you never try to immediately lift or remove the gauze without proper preparation. Instead, pour warm, clean water and saline solution over the entire affected area and let it sit for several minutes.
Ensure that the area is moist—not wet. Too much moisture can lead to maceration, in which the skin becomes too soft, and the barrier becomes damaged. As you moisten the gauze, it softens dried fluids and loosens adhesion, making removal seamless and pain-free.
Step 3: Gently Lift the Gauze—Do Not Pull
Once you feel the gauze has loosened, begin slowly peeling it off one corner at a time. It’s crucial to go extremely slowly during this process, as any resistance can damage the injury. Lift one corner and stretch it horizontally along the skin, avoiding pulling straight up. Additionally, gently place a finger on the dressing itself to keep it taut during removal.
If you do notice the gauze isn’t coming off easily, pause and re-saturate the area. While some opt for petroleum jelly or similar lubricants, we recommend avoiding this if possible. Petroleum jelly is not an official antiseptic and can further trap bacteria, irritate the wound, and result in maceration.
Step 4: Clean the Wound After Removal
Once you have successfully removed the gauze, clean the wound with appropriate cleaning agents as directed by medical guidelines. Be sure to avoid harsh antiseptics, such as hydrogen peroxide or alcohol, as they can damage healthy tissue, slow wound closure, and dry out the wound bed.
Instead, ensure you use antimicrobial ointments and prescribed treatments and apply from the center of the wound outward. These formulas are specifically designed to target harmful bacteria and microorganisms that can hinder recovery.
Step 5: Apply the Appropriate Dressing
After thoroughly cleaning the wound, put on new, fresh gloves and pat the skin dry. Now, apply the appropriate dressing depending on the wound type. The right dressing will help prevent the gauze from sticking again and protect the wound as it continues to heal.
Here is a simple breakdown of the most common types of wound dressings:
Non-Adherent Gauze: Either silicone-based or made with soft paraffin, non-stick, non-adherent gauze features a non-stick film. This allows for gentle removal and is ideal for burns, post-surgical incisions, or skin grafts.
Antimicrobial Dressings: Infused with either silver, iodine, or honey, this dressing acts as a barrier to prevent microbes and disrupt bacterial cell walls. They’re ideal for managing chronic wounds, pressure ulcers, and heavily contaminated wounds.
Transparent Film: This clear dressing allows patients or caregivers to directly monitor skin while still protecting it. They’re not absorbent, so they typically work well to secure additional dressings.
Alginates/Hydrofibers: Highly-absorbent dressings made from natural sources, alginate and hydrofiber promote debridement and help reduce pain. Due to their soft gel, they work well for venous ulcers, diabetic ulcers, and tunneling wounds with sinus tracts.
Foam Dressings: These dressings are absorbent, cushioned, and made of polyurethane to protect healing skin and maintain a moist wound environment. Because foam dressings add cushion to fragile areas, they’re ideal for pressure injuries and diabetic foot ulcers.
Hydrocolloids: This adhesive dressing has a gel-forming inner layer that promotes quicker healing and efficiently absorbs exudate. They’re waterproof and flexible, making them well-suited for burns, abrasions, surgical wounds, and pressure ulcers.
Hydrogels: These water-based gel dressings feature 90% hydrophilic polymers that support autolytic debridement, moisture balance, and pain relief. They’re particularly effective for burns, abrasions, pressure ulcers, and diabetic ulcers.
Related: How Long Does a Tunneling Wound Take to Heal?
Step 6: Monitor for Signs of Infection
After cleaning and applying the new dressing, watch for signs of infection as the wound continues to heal. Physical symptoms include redness, warmth, swelling, pain, drainage, and wound reopening. Systematic symptoms, on the other hand, can include fever, swollen lymph nodes, chills, body aches, or weakness.
Early intervention is essential for proper treatment and management. The sooner you can catch a potential infection, the better you can avoid complications and recover successfully.
Step 7: Visit a Wound Care Specialist for Additional Help
Whether you’re experiencing difficulty removing gauze or you’re managing complications with a wound, visit a wound care clinic. Here, trained and certified specialists can swiftly diagnose, treat, and continue monitoring the area.
Additionally, specialists, such as those at Royal Wound Care, are committed to delivering exceptional, accessible care through advanced wound treatments, personalized care plans, and versatile service options. If you’re looking for faster healing and proven wound care solutions, consider:
Common FAQs About Gauze Stuck to Wounds
How do I stop gauze from sticking to a wound?
Preventing gauze sticking is often easier than managing after the fact. A few active steps can significantly reduce discomfort and protect healing tissues:
Ensure you use a non-adherent dressing layer before applying the gauze. These dressings often contain silicone or a special coating to protect the skin and make changes less painful.
Keep the wound slightly moist—not wet. Avoid submerging it entirely or adding too much saline solution at once. However, research shows that a moist environment is essential to optimal wound healing—so it’s essential not to skip this step.
Avoid allowing the gauze to dry directly onto the wound. Do this by applying a moisture-retaining layer, like antibiotic ointment, and moistening stuck gauze with warm water or saline solution.
Choosing high-quality dressing materials and following proper techniques reduces the likelihood of gauze sticking to a wound and delaying recovery.
How often should I change my gauze?
The frequency of dressing changes depends on the type of wound, the amount of drainage, and the medical guidance. However, gauze changes typically follow this timeline:
Minor cuts or scrapes: Daily when it gets wet, damaged, or dirty
Lightly draining wounds: Can last for multiple days, or even a week, if there isn’t a large amount of exudate
Moderately draining wounds: A few days maximum, but needs to be changed after it becomes soiled
Heavily draining wounds: Generally need to change multiple times a day to manage moisture and reduce the likelihood of sticking
Regular dressing changes reduce the risk of infection, help prevent the gauze from sticking, and allow you to monitor the healing progress. Most importantly, follow your physician’s guidance while caring for your wound.
Can you soak gauze off a wound?
You can absolutely soak gauze off a wound. However, it’s important to do this process mindfully. Using warm water and saline, gently pour the solution over the gauze and edges of the dressing. Allow it to sit for several minutes before trying to remove it. Unless necessary, avoid submerging the wound or leaving it wet for extended periods. Doing so may cause maceration, disrupting the normal healing process and leading to complications.
Should you remove stuck gauze when it’s dry?
Absolutely not—avoid removing dry gauze if it is stuck to a wound. Doing so may pull off new, fragile tissue. As a result, this can cause intense pain, re-injury, bleeding, and potential infections. Ultimately, this disrupts the recovery process and makes it harder to remove the remaining gauze.
If you’re having trouble, visit a local wound care facility or your physician for additional help.
With the right techniques, you can safely and successfully remove gauze stuck to a wound without pain or irritation.
Gauze sticking to a wound can be stressful—especially when it comes to minimizing pain and reducing tissue damage. However, with proper techniques, patience, and the right materials, it is entirely possible to effectively remove the gauze without delaying recovery. By understanding why gauze sticks to a wound and knowing when to act, you can support healing and promote optimal recovery.
Wound healing can often feel both isolating and overwhelming. This is why at Royal Wound Care, we prioritize creating a better care experience, where patients receive the treatment they deserve. Don’t hesitate to contact the Royal Wound Care team if you or a loved one are struggling with recovery.
For SNFs and independent nurses, visit our site to review our educational opportunities and professional partnerships. From faster healing times and lower infection rates to fewer wound-related hospitalizations and lower facility costs, we ensure professionals have everything they need to advance care and treatment. Partner with Royal Wound Care to bring expert-level bedside wound management to your facility today!
Request an Appointment at a Royal Wound Care Facility near you.
Royal Wound Care is the expert in wound healing. Our board-certified wound care specialists are ready to help you begin your healing journey. Click the button below to request an appointment at a Wound Care Center near you—no referral needed
© 2025 Royal Wound Care, LLC. All rights reserved.
site by Growth Partners Marketing

