Chronic Wounds: When Healing Stalls
Chronic wounds are wounds that don't heal in the expected timeframe, often taking weeks or even months. Unlike acute wounds that follow a predictable healing process, chronic wounds get stuck due to various underlying factors.
Find Wound Care Near You
If you or a loved one is struggling with a wound that won’t heal, a Royal Wound Care Wound Care Center can help. Since there is no need for a referral, your treatment is only a click and call away.
Common Causes:
Vascular Disease: Poor blood circulation can deprive tissues of oxygen and nutrients.
Diabetes: High blood sugar can impair wound healing.
Pressure Injuries: Prolonged pressure on the skin, often in immobile patients.
Infection: Persistent infection can hinder the healing process.
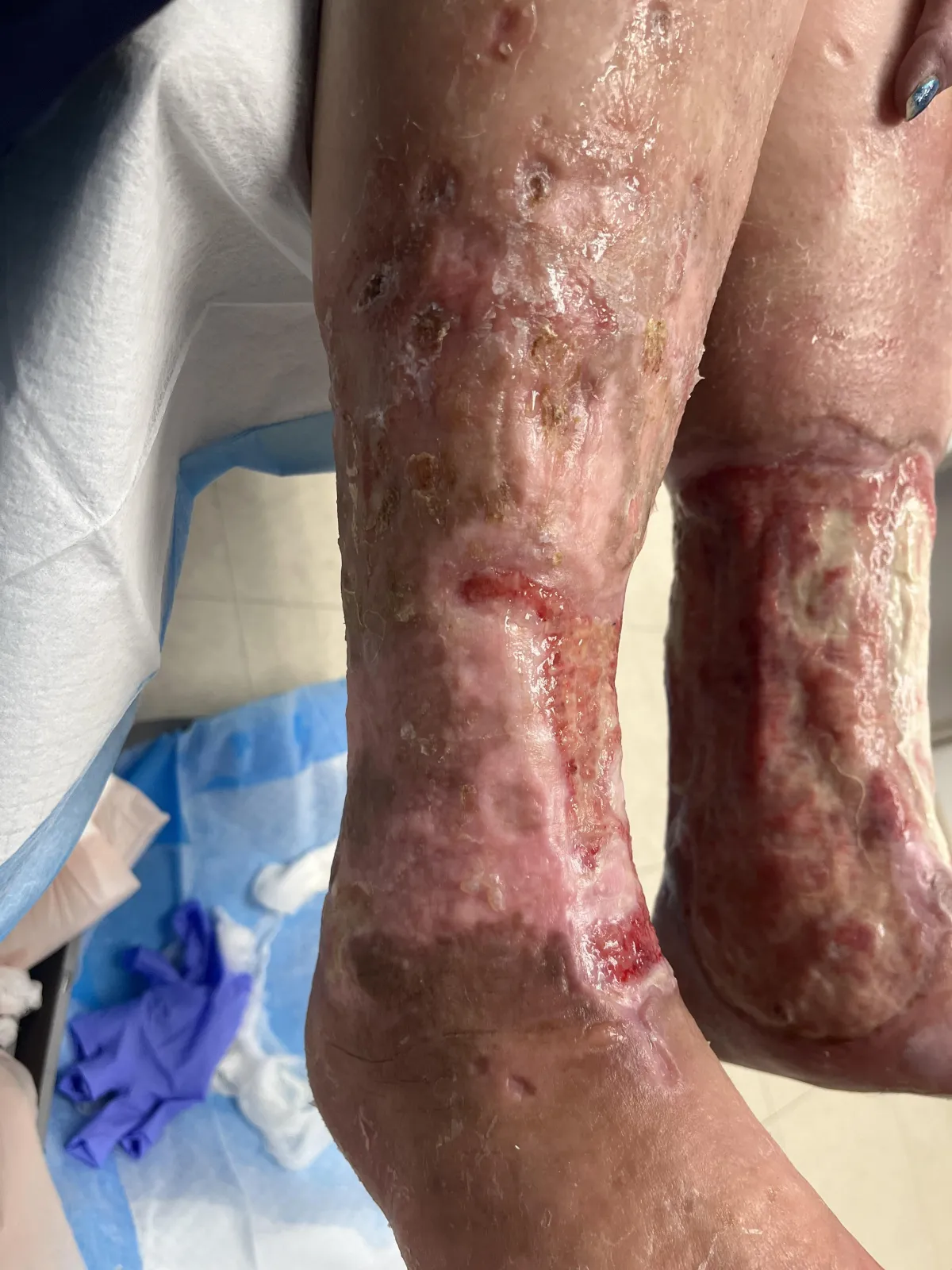
If you have a wound that isn't healing, seek medical attention. Proper wound care and addressing the underlying cause are crucial for healing.

The Impact of Heart Health on Wound Healing
1 in 2 Americans suffer from a cardiovascular disease. Coronary artery disease, peripheral artery disease and other issues with the heart and vessels can cause blockages that obstruct the flow of blood.
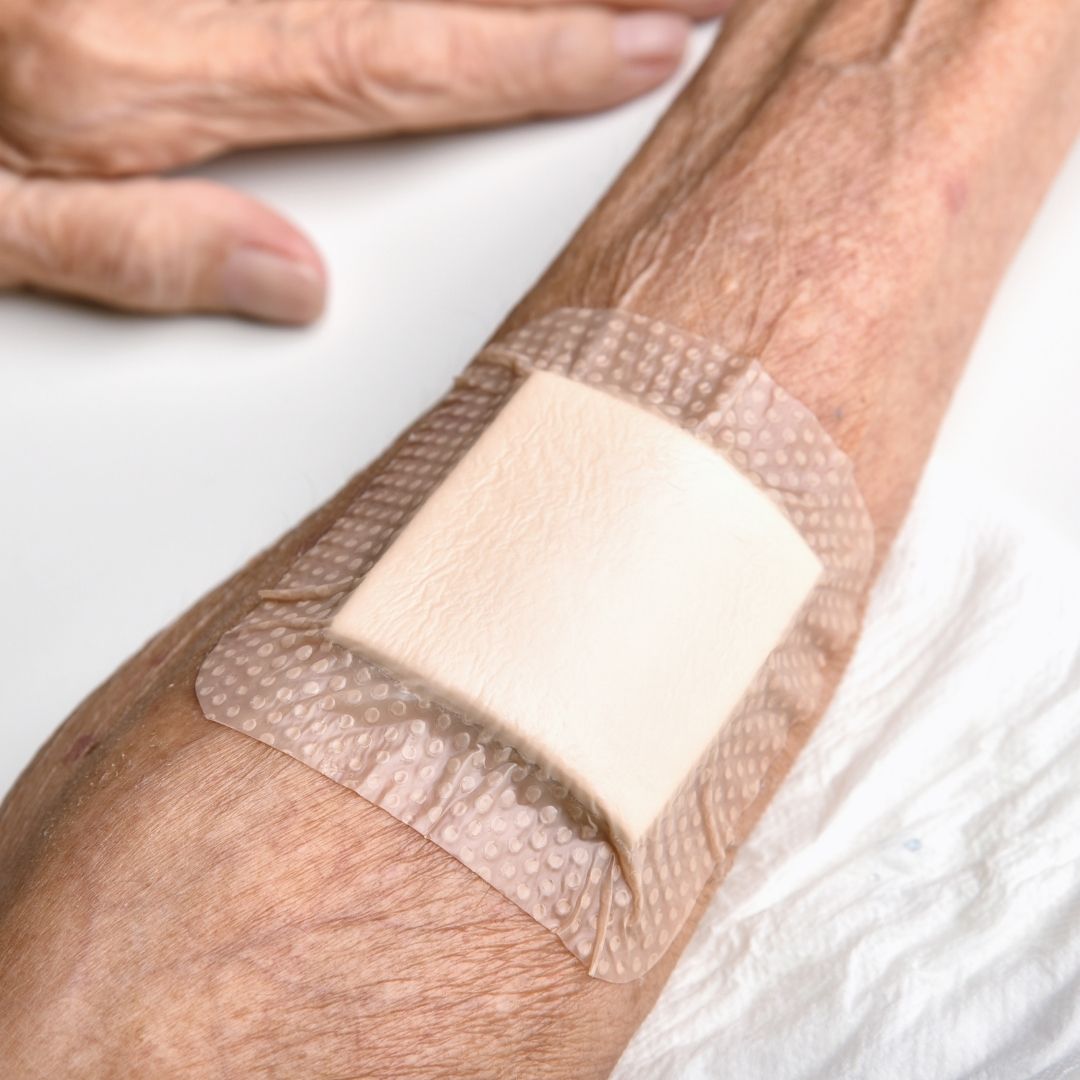
8 Types of Foam Dressings and When to Use Each One
8 Types of Foam Dressings and When to Use Each One
Dressings are essential in modern wound care, and foam dressings are among the most efficient options. Due to their impressive combination of absorption, cushioning, moisture balance, and protection in a single dressing, they’re ideal for both acute and chronic wounds.
However, as we mentioned in “Dressings for Pressure Sores,” foam dressings are a single branch of the broader wound care toolkit. While they share similar core benefits, there are various types of foam dressings designed to manage different injuries. Differing in material, absorption capacities, and adhesion, it’s important to understand how to tailor dressing options to individual needs.
In this guide, we discuss the different types of foam dressings and when to use each specific one. We will explore what foam dressings are, what they’re typically used for, and how to apply them properly. Whether you’re an RN caring for inpatient injuries or someone treating their wound with home health care, this knowledge is crucial for optimal recovery.

8 Types of Foam Dressings and When to Use Each One
While foam dressings share core functions, they vary greatly in design. And at Royal Wound Care, where comprehensive, focused treatment is foundational, these seemingly minor details make all the difference.
Ultimately, no two injuries are the same. While two patients may both be dealing with tunneling wound recovery, their lifestyle factors, genetics, age, and pre-existing conditions all play a significant role in recovery. Similarly, foam dressings differ in sustainability, comfort, wear time, and clinical effectiveness.
These factors can influence how well a dressing manages moisture, stays in place, and minimizes pain during removal. To abide by best practices, understanding the differences in foam dressings is essential. Additionally, this information can help clinicians, caregivers, and individuals choose the most appropriate option for their unique circumstances.
What Is Foam Dressings for Wounds?
Foam dressings are polymer-based absorbent wound dressings made with small, open cells that allow them to absorb and retain wound fluid (exudate). As we know from modern research, a moist wound environment facilitates the healing process. It reduces tissue dehydration, cell death, and, equally as important, pain during healing.
Foam dressings facilitate this process by drawing exudate away from the wound bed without drying it out. More specifically, the semi-permeable film removes exudate while the hydrophobic backing prevents leakage, creating a humid, warm environment. This moisture-balancing approach maintains an optimal environment while protecting surrounding skin from maceration.
In addition to absorption, foam dressings also provide:
Cushioning and protection. With a thick, porous structure, foam dressings protect wounds against pressure, friction, and shear forces.
Thermal insulation. Foam dressings trap air, creating a barrier between the wound and the external environment. This is crucial, as cold temperatures can slow wound healing.
Non-adherent surfaces. While some foam dressings feature adhesive borders, they do not have adherent surfaces. This allows the dressing to rest against the wound bed without sticking to the healing tissue, minimizing pain during removal.
Bacteria protection. As a protective layer, foam dressings help prevent bacteria and external contamination from entering wounds. This reduces the risk of infection, physical trauma, and re-injury.
Related: How to Remove Gauze Stuck to Wound Without Pain: Step-by-Step
What Are Foam Dressings Used For?
Because foam dressings are absorbent and cushioning, they’re best for wounds with heavy-to-moderate wound exudate and sensitivity to pressure. For example, foam dressings are commonly used in the management of:
Pressure injuries (stage II–IV)
Surgical incisions and post-op sites
Traumatic or abrasion wounds
Donor sites or cavity wounds
As protective padding over bony prominences and high-friction areas

Different Types of Foam Dressings
Adhesive Foam Dressings
Adhesive foam dressings are breathable products that feature a built-in adhesive layer to secure around the surrounding skin. Additionally, adhesive foam dressings are often referred to as “island dressings” due to their central pad and adhesive tape border.
Adhesive foam dressings are ideal for:
Flat or shallow wounds
Wounds that require consistent coverage
First- and second-degree burns
The design allows for seamless application without the need for additional tape, wrap, or secondary fixation. Moreover, this type of foam dressing is particularly convenient and time-efficient.
Non-Adhesive Foam Dressings
Non-adhesive foam dressings are soft pads that absorb wound exudate without sticking to the wound bed. Unlike adhesive dressings, however, this option does not feature a sticky layer. Instead, you must secure it with secondary fixation such as gauze, tape, or compression wraps.
Non-adhesive foam dressings are ideal for:
Joint areas, like elbows or knees, that experience frequent movement
Patients with sensitive skin or wounds
Wounds where adhesive may cause skin stripping
Suitable for atraumatic dressing changes, non-adhesive options prevent damage to healing and periwound skin. Additionally, they’re highly versatile, making them safe for injuries from pressure ulcers to skin tears.
Silicone Foam Dressings
Silicone foam dressings feature a soft pad and a gentle silicone adhesive layer that sticks to surrounding skin without adhering to the wound bed. Both breathable and waterproof, the foam absorbs and retains exudate while minimizing pain during removal.
Silicone foam dressings are ideal for:
Patients with fragile, sensitive, or aging skin
Elderly patients
Wounds requiring frequent dressing changes
Silicone foam dressings are especially effective in situations where comfort and skin protection are equal priorities, as they promote healing and conform comfortably to the body.
Hydrocellular Foam Dressings
Hydrocellular foam dressings are made of polyurethane foam to maintain moisture and provide non-adherent cushioning. A more advanced option, the layered structure absorbs fluid and distributes it horizontally across the dressing. As a result, this reduces pooling and leakage.
Hydrocellular foam dressings are ideal for:
Venous leg ulcers
Surgical wounds
Heavily draining pressure injuries
Additionally, because they’re so flexible, they seamlessly conform to body contours without lifting, tearing, or stretching.
Antimicrobial Foam Dressings
Antimicrobial foam dressings, made of polyurethane foam, silver salts, cadexomer iodine, and additional antiseptic agents, help manage bacteria in the wound. In addition to reducing bacterial bioburden for up to 7 days, they also manage moderate-to-heavy wound exudate and provide comfort.
Antimicrobial foam dressings are ideal for:
Infected wounds
Wounds with delayed healing due to bioburden
Chronic ulcers
It’s important to use this dressing type under the guidance of a clinician or wound specialist. Because they absorb moisture so effectively, they can dry the wound bed and hinder healing.
Foam Dressings with Border
Foam dressings with a border feature a wide adhesive perimeter to enhance seal and reduce leakage. With an absorbent pad and a silicone or acrylic adhesive pad, they’re particularly effective for protecting healing environments without the need for secondary tape.
Foam dressings with a border are ideal for:
Limbs or torsos
Heels and around joints
High-movement areas where secure placement is essential
Compared to other foam dressings, those with a border offer an all-in-one solution. Additionally, they maintain a moist healing environment and ensure the dressing remains in place.
Cavity or Shaped Foam Dressings
Cavity- or shaped-foam dressings are specifically designed to manage deep or irregularly shaped wounds with moderate-to-high exudate levels. Due to their flexibility, clinicians and caregivers can easily cut and fold the dressing to fit injuries comfortably.
Cavity or shaped foam dressings are ideal for:
Pressure injuries
Deep, tunneling wounds
Cavity wounds with “dead space”
At times, depending on the severity and depth, cavity- or shaped-foam dressings require packing. Doing so ensures bottom-up healing, preventing wounds from first healing at the surface and leading to complications.
High-Absorbency Foam Dressings
High-absorbency foam dressings feature an enhanced core that manages heavy-to-extremely heavy exudate. Even under compression, the high-absorbency foam balances fluid and retains it without leaking, tearing, or increasing the risk of maceration.
High-absorbency foam dressings are ideal for:
Wounds with excessive drainage
Injuries for which extended wear is beneficial
Pressure wounds
Additionally, high-absorbency dressings are often multilayered. As a result, they improve patient comfort and offer greater capacity.

How to Use Foam Dressing for Wounds
Assess Exudate Level Before Selecting Dressing
Before choosing a foam dressing, assess the injury to measure the amount of wound exudate. Wounds with large surface areas or significant depth, for example, require specialized, highly absorbent solutions. Matching absorption capacity to fluid levels is key for preventing leakage, maceration, and potential dryness.
Related: Royal Wound Care At Home: A Nurse’s Step-by-Step Checklist
Avoid Foam Dressings on Dry, Non-Draining, or Necrotic Wounds
Foam dressings require moisture to function properly, as this is what promotes faster healing and prevents cell death. However, if the wound is dry, the dressing will simply adhere to the wound bed. As a result, it can cause significant pain, skin tearing, and additional desiccation. It’s vital to only apply foam dressings to wounds that produce exudate.
Protect the Periwound Skin
Periwound skin, the environment immediately surrounding a wound, is critical in wound care. However, it’s often overlooked in individuals caring for wounds at home, as many don’t know how significant it is to healing.
Protecting the periwound skin prevents skin breakdown, adhesive trauma, and wound enlargement. During dressing changes and removal, ensure you follow proper methods to avoid additional trauma.
Select Adhesive or Non-Adhesive Foam Based on Skin Integrity
There is no such thing as the “best” dressing, as each option offers specific, unique benefits. The best option is the one that promotes healing and ensures the patient remains comfortable. A major component of this decision relies on skin integrity.
Patients with fragile, elderly, or sensitive skin may benefit more from a non-adhesive foam dressing. This can reduce the likelihood of additional trauma and adhesive-related skin stripping (MARSI).
Monitor Wear Time
Most patients can safely leave foam dressings on for 3–7 days. However, this timeline relies significantly on wound severity, clinician recommendations, and manufacturer instructions. For dressings that leak, lift, or become soiled, it’s important to change them immediately. Leaving it on for an extended period of time can promote bacterial growth and increase the risk of infection.
Cut Foam Dressings to Fit Wound Shape
For cavity or irregular wounds, trim foam dressings to fit comfortably. To do this, measure the longest length and the widest width of the wound. Additionally, it should fit around 1–2 cm larger than the wound area.
A successful application will cover the wound bed without overlapping on healthy skin too much. Also, don’t forget: rub the edges gently after cutting to remove any loose particles or debris.
Ensure Dressing Remains Fixed in High-Movement Areas
It’s important to ensure the dressing adheres to the proper area regardless of wound type. However, high movement areas are particularly susceptible to shifting, peeling, and lifting.
Ultimately, this can lead to delayed healing or infections by exposing the wound to contaminants. Keep a close eye, especially after periods of frequent movement. If the dressing shifts, safely and gently replace it.
Reassess Dressing Choice as Wound Heals
As wounds progress and exude levels change, the type of foam dressing should as well. As we mentioned previously, foam dressings aren’t effective on dry wounds and can ultimately result in prolonged damage. Reassess conditions throughout healing and change dressing types as needed.
Foam dressings are an essential component of modern wound care, promoting optimal healing outcomes when selected appropriately.
Dressing type, as we’ve discussed throughout this post, is one of the many crucial components in optimal healing. With the proper education and clinician-led recommendations, patients and caregivers can make informed decisions that support healing and reduce complications.
At Royal Wound Care, our highly trained team prioritizes reducing infections and achieving optimal healing outcomes. From in-clinic wound care services to mobile wound care, we don’t just treat the wound—we treat the patient as a whole, wherever they are in their healing journey. If you or a loved one has any questions, don’t hesitate to contact Royal Wound Care today!
For SNFs and independent nurses, make sure to visit our site and learn about our educational opportunities and professional partnerships. Healing shouldn’t feel complex, confusing, or inaccessible—and with the right team, it doesn’t have to be. Reach out to our team today to learn more about how you can advance your career or clinic with hands-on training and expert-level precision.
Request an Appointment at a Royal Wound Care Facility near you.
Royal Wound Care is the expert in wound healing. Our board-certified wound care specialists are ready to help you begin your healing journey. Click the button below to request an appointment at a Wound Care Center near you—no referral needed
© 2025 Royal Wound Care, LLC. All rights reserved.
site by Growth Partners Marketing
