
Royal Wound Care: Among the nation’s few board-certified wound care clinics
From initial wound diagnosis through resolution, Royal Wound Care provides the highest level of wound management throughout the skilled nursing facilities we serve. Providers in all locations are trained extensively on evidence-based clinical guidelines, with wound care nurses and specialty physicians medically following the patient during transitions of care.
For questions regarding our skilled nursing facilities, please book an appt here.
We improve patients’ lives through research.
Since our founding, Royal Wound Care has made optimal wound care accessible to all by combining cutting-edge research with a highly trained, board-certified staff. We’ve published peer-reviewed articles, shared expert-led webinars, and partnered with leading academic and advocacy organizations to advance the field of wound healing. Click the link below to explore the latest in wound care news and access insights drawn from our extensive clinical experience.
Through wound science and research, we are helping to heal more wounds.
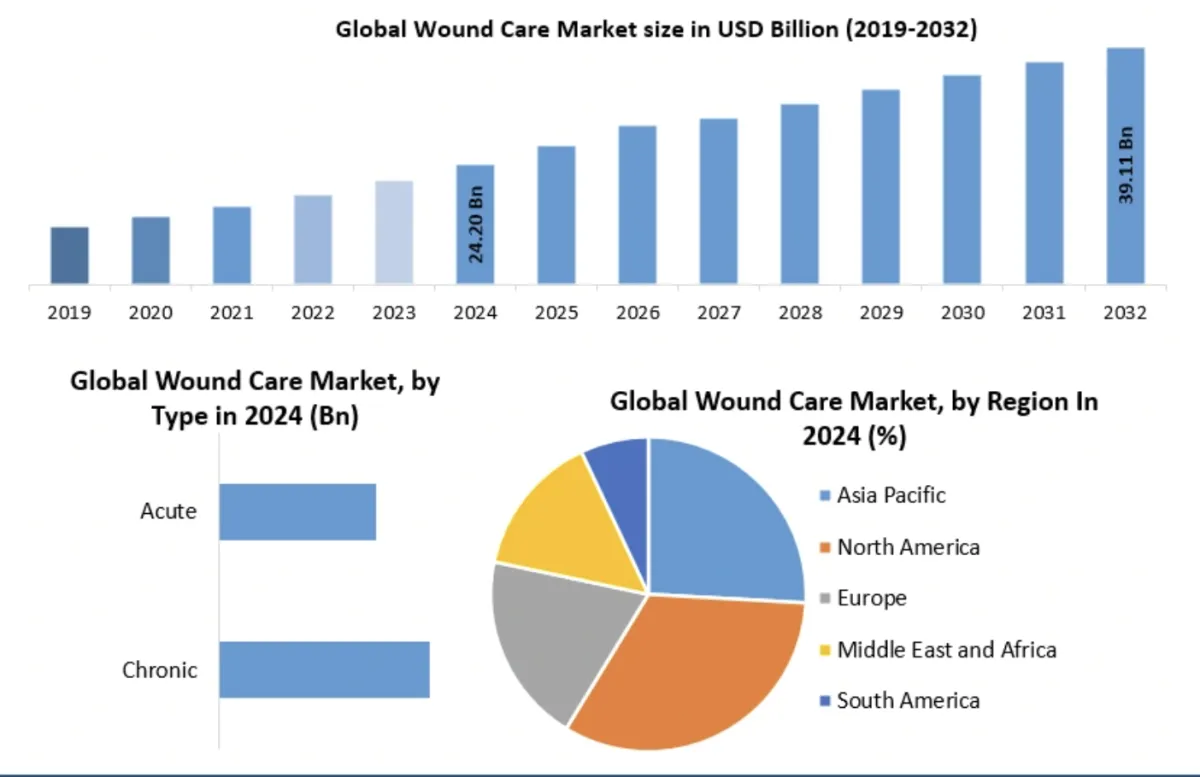
More Data, More Knowledge
The more we examine wounds, the better we understand how ulcers develop and progress into more serious wounds.
Partnerships for Increased Insight
By collaborating with academic and scientific experts, we integrate external research with our clinical insights to better understand what makes certain treatments effective—and why others fall short.
Working Toward Wound Prevention
While modern wound care has helped millions heal, our ultimate goal is to one day predict and prevent ulcers before they develop into chronic wounds.
The latest in wound care.
In a recent update from Royal Wound Care , our medical team highlights concerning trends in major limb amputations, noting a significant increase during the COVID-19 pandemic compared to pre-pandemic periods. These findings emphasize the critical need for early intervention, consistent wound care, and ongoing patient education—especially during times of healthcare disruption.
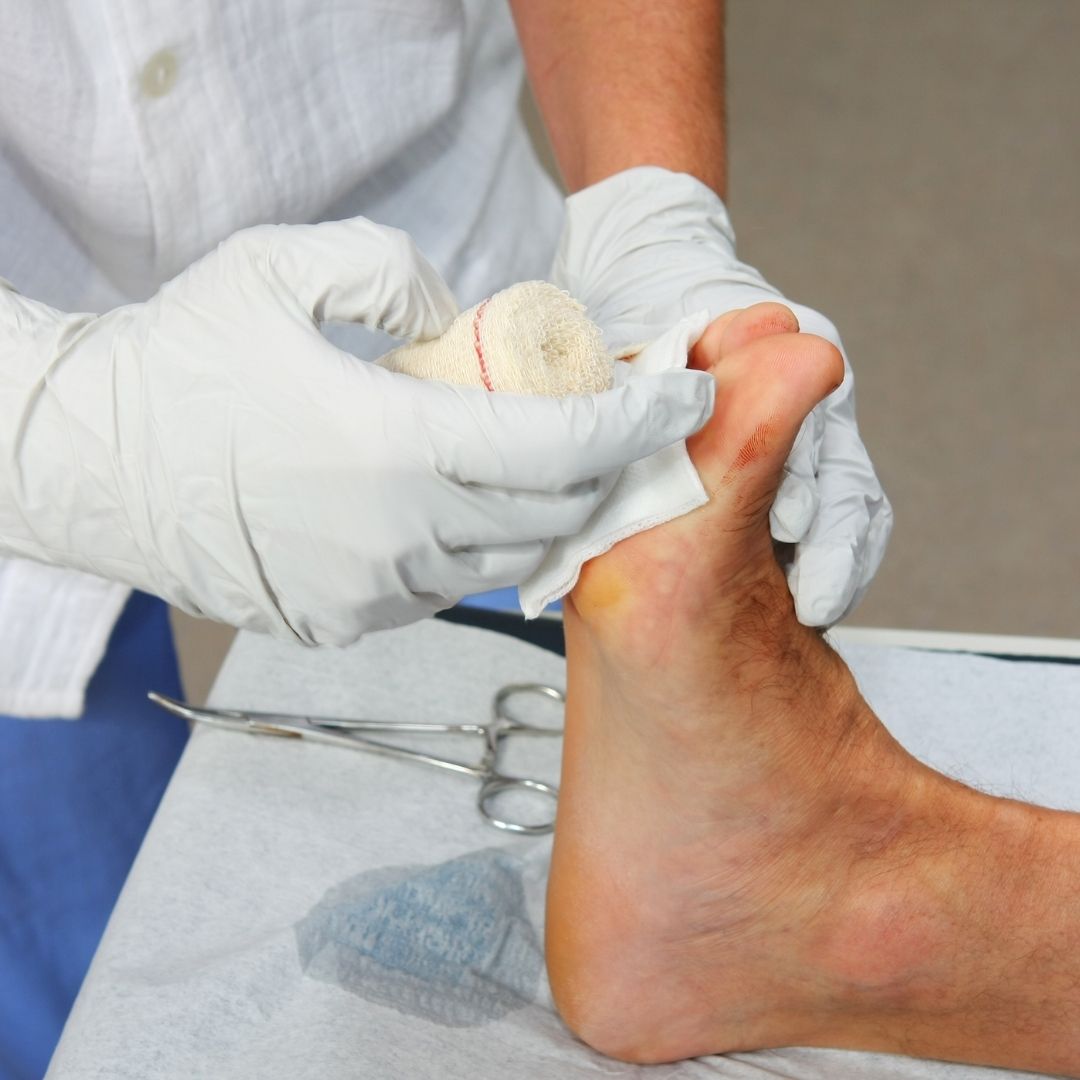
Skin Prep for Wound Care: Best Practices for Proper Healing
Skin Prep for Wound Care: Best Practices for Proper Healing
In wound care, there are many moving parts to ensure safe, optimal healing. Skin prep is a critical—and often overlooked—first step in the process. Before applying dressings, the periwound skin must be prepared to support cleaning, secure adhesion, and prevent infection. Skin prep is an important tool for this process.
Dressings and medical adhesives must stay in place to protect open wounds and manage wound drainage. Without preparation, patients may experience tape stripping and friction, discomfort during adhesive removal, or even skin injury. We recently discussed this in our guide, “How to Remove Gauze Stuck to a Wound.”
To maintain an optimal healing environment, understanding how to care for wounds is the first, most important step. Therefore, in this guide, we will discuss what skin prep is, why it matters for wound healing, and a step-by-step approach for application. We’ll also cover key safety considerations important for both clinical and home health care settings.

Skin Prep for Wound Care: Best Practices for Proper Healing
Skin prep is far more important than simply helping wound dressings stick. It’s the process of reducing the microbial load, protecting the skin from irritation, and creating an optimal surface for dressing application—all factors crucial in proper healing.
Additionally, prioritizing skin prep can significantly improve how well dressings and medical devices adhere to the skin without causing trauma, tearing, or discomfort during changes. This is particularly important for complex wounds that require frequent removal.
In this post, you can find:
What skin prep is for wounds, and its role in healing
The differences between skin prep and wound cleansing
When you should use skin prep in wound management
A step-by-step guide for proper application
Common mistakes and best practices
How to integrate skin prep into home wound care management
At Royal Wound Care, we believe it’s helpful to know not only what steps to take in wound management, but why each one matters. That’s why this patient-focused resource is designed to be educational, supportive, and rooted in evidence-based practices.
What Is Skin Prep for Wounds?
Skin prep for wounds is a clinical method used to protect the skin surrounding a wound site. Think of it as a shield for the wound bed, protecting the injury against trauma, excessive moisture, bacteria, and friction. There are also many different types of skin prep products, including:
No-Sting Barrier Films: These alcohol-free, liquid-based formulas form a protective barrier over periwound skin. They’re breathable, transparent, and waterproof, protecting the area from friction and adhesive trauma.
Adhesive Preps and Barriers: Often in the form of sprays, wipes, or foams, these products are applied before adhesive application. It creates a gentle, tacky layer that helps medical devices and dressings stick securely while also shielding the wound.
Skin Protectants: These barrier agents are typically available as creams, liquid films, wipes, or sprays. A patient or caretaker will apply it to periwound skin to reduce moisture loss and protect injuries from adhesive stripping. They are often transparent and silicone-based, specialized for sensitive skin.
Many reputable companies, such as Smith & Nephew, formulate their products to be durable, breathable, protective, and long-lasting. However, skin prep should be used only on intact skin, not applied directly to open wound beds unless specifically directed otherwise by a clinician.
Related: Caring for Your Wound

What Does Skin Prep Do for Wounds?
Skin prep offers many functional benefits when caring for wounds, including:
Removes Oils, Dirt, and Residue
Before applying skin prep, it’s crucial to cleanse, sterilize, and dry the area. Otherwise, bacteria, oil, dirt, and residue remain trapped underneath the dressing, increasing the risk of infection and slow healing.
After cleansing, skin prep forms a fast-drying, sterile barrier that prevents irritants from reaching the wound bed. Additionally, this process ensures that adhesive dressings bond securely to the injury site, fully protecting it.
Related: Avoiding Common Wound Care Mistakes
Protects Periwound Skin From Irritation and Trauma
When changing dressings, it’s not uncommon to experience irritation. However, whether due to frequent changes or improper application, adhesive removal can damage healthy skin and lead to skin tearing. When this happens, it significantly complicates the healing processes and increases the risk of infection.
Fortunately, skin prep helps protect healthy skin by creating a non-oily barrier film, ultimately maintaining skin integrity. Dressing removal becomes an easy, painless process that doesn’t result in cumulative damage.
Forms a Breathable, Waterproof Barrier
Recent research demonstrates that keeping wounds moist is essential for proper healing. However, they should never be excessively moist, as this increases the risk of maceration—a condition that causes skin damage due to overly soft tissue.
By providing a protective barrier, skin prep keeps necessary moisture within the dressing while keeping contaminants, such as sweat, ostomy effluent, or wound drainage out. Still, it remains breathable, allowing water vapor to pass through and avoiding maceration risk entirely.
Additionally, some products like SKIN-PREP® Protective Dressing are designed to be long-lasting, hypoallergenic, and flexible, prioritizing both efficiency and safety.
Improves Dressing Displacement
Many patients experience dressing displacement—especially those in long-term care or individuals navigating chronic wound management. When using skin prep, however, the tacky layer improves dressing attachment and enhances adhesion.
Additionally, it smooths out minor skin contours that may otherwise influence how a dressing remains on the surface. By ensuring that the dressing does not slip, move, or slide, patients can better reduce the risk of bacteria reaching the wound and negatively impacting healing.
Skin Prep vs. Wound Cleaning
Although wound care specialists will discuss these two processes together, skin prep and wound cleaning serve different purposes.
Skin prep targets intact periwound skin. This is the area surrounding the wound bed—the skin that the adhesives will directly touch. When clinicians discuss “skin prep,” they are referring to a specific product that forms a protective barrier over an injury. This essential tool reduces surface bacteria while helping dressings and medical devices adhere better.
Wound cleansing, on the other hand, is the process of removing debris inside the wound bed using gentle cleansers and antimicrobial ointments. When managing wounds at home, it’s important to note that clients should avoid using harsh antiseptics. Products such as hydrogen peroxide and alcohol can damage healthy tissue and slow wound closure.
Both steps are essential components of comprehensive care and long-term recovery.
Related: Wound Care at Home: A Nurse’s Step-by-Step Checklist
Step-by-Step Skin Prep for Wound Care
The team at Royal Wound Care believes that treatment should be personalized, compassionate, and accessible. Even though it may seem complex, skin prep is straightforward with the proper guidance and supplies.
Below is a simple, step-by-step guide for effective skin prep:
Step 1: Wash hands. Before touching the wound, wash your hands thoroughly. Doing so removes any germs and bacteria that you can easily transmit to the injury. Afterwards, apply latex gloves for additional protection.
Step 2: Clean and dry wound. Using mild soap and water or saline solution, gently cleanse the wound. The skin should feel cool or slightly warm. Afterwards, pat it dry with a sterile cotton cloth.
Step 3: Apply skin prep. Apply the skin prep evenly to intact skin surrounding the actual wound. Make sure you avoid applying it directly to the open wound unless directly advised by your physician. Doing so may compromise tissue integrity, damage delicate skin cells, and delay healing.
Step 4: Allow product to dry. Before applying the dressing, let the skin prep dry for at least 30 seconds. This ensures that the skin fully absorbs the product and creates a smooth base. Additionally, it’s essential for barrier integrity and proper dressing or device adhesion.
Step 5: Apply dressing or adhesive device. After 30 seconds, the skin prep should feel slightly tacky or sticky. This means you are doing everything correctly! Now, apply the dressing or adhesive device, smoothing the border to ensure it’s sealed properly.
Step 6: Reapply. Next time you remove the dressing or medical device, make sure you reapply skin prep as well. The product will not stay on the skin with proper cleansing.
Best Practices and Safety Tips
Patch test new skin-prep products before applying them to periwound skin.
Before applying skin prep products, make sure you patch-test them in a discreet but accessible area. This step is particularly important for individuals with sensitive skin. Doing so prevents adverse reactions—most commonly contact dermatitis, hives, rashes, or eczema flare-ups.
Test the product on clean, dry, and easily accessible skin—such as the area behind the ear, elbow, or forearm. Afterwards, monitor the area for 48–72 hours to ensure there are no adverse reactions. If you experience itching, dryness, irritation, or redness, remove the product and avoid applying it to periwound skin.
Avoid using strong alcohol or peroxide directly on wounds.
As we mentioned earlier, patients and caregivers should avoid using harsh antiseptics on wounds. Although once popular in wound healing, these cleansers are considered cytotoxic agents, substances that damage skin cells crucial to healing.
Unless your wound care specialist has directed otherwise, clean the wound with warm water and a gentle soap or saline solution.
Do not apply skin prep on open wound beds—only on intact periwound skin.
Skin-prep is specifically formulated for healthy, intact skin. Applying it to wound beds is highly discouraged and can be harmful both to the wound and the healing process. For example, patients who apply skin prep directly to a wound may experience tissue damage, irritation, and increased inflammation.
If skin prep does accidentally reach the wound bed, cleanse the area with saline solution immediately. If you need additional help, contact the team at Royal Wound Care. We’d be happy to treat or assist you through the process.
Use sterile techniques as appropriate to your setting and wound type.
Different types of wounds require different techniques necessary for healing. Treatment for minor lacerations, for example, will be much more straightforward than healing a tunneling wound. Because of this, it’s important to follow the appropriate sterilization methods for your wound type.
Chronic or complex wounds often use advanced wound treatments and frequent dressing changes. Diabetic foot ulcers, on the other hand, require careful offloading and specialized dressing management. Using improper methods may not effectively treat the wound, making healing more difficult.
Coordinate with clinicians for infected or complex wounds.
For those managing complex or infected wounds, we recommend contacting a certified wound care specialist. These professionals can successfully assess wound severity, recommend appropriate treatment options, and help prevent complications.
Additionally, the right team, like those at Royal Wound Care, will ensure you feel supported from diagnosis to resolution. Visit our page, “Board-Certified Wound Care,” to learn more about how physicians improve lives and reduce hospitalizations.
Skin Prep for Wounds
We briefly discussed different skin prep products for wounds earlier. However, this comprehensive section will provide additional information about what each product is ideal for:
Barrier Films and Sprays
Barrier films and sprays are ideal for protecting at-risk periwound areas and sensitive skin. By forming a protective, breathable, water-resistant barrier, this skin-prep product preserves skin integrity during healing. Additionally, it minimizes the risk of adhesive trauma during dressing changes or device removal.
Common uses of barrier films and sprays include:
Preventing medical adhesive-related skin injuries (MARSI)
Managing incontinence-associated dermatitis
Protecting the skin around a stoma from wound exudate
Reducing friction between high-risk, fragile, or sensitive skin
Prep Wipes/Pads
Prep wipes and pads are extremely convenient for quick application before putting on bandages, dressings, or medical devices. They form a waterproof, gentle barrier against periwound skin, are fast-drying, and adjust well to high-friction areas without peeling or cracking.
Common uses of prep wipes and pads include:
Securing tapes and dressings around a wound
Preventing irritation from catheter sites
Shielding skin from ostomy effluent
Preparing skin for Wound VAC Therapy (Negative Pressure Wound Therapy)
Alcohol-Free vs. Alcohol-Based Preps
Alcohol-based skin-prep products are generally ideal for situations where patients require a quick, high-level disinfection. Common examples include injections or blood draws. They’re fast-drying, leave no residue, and sanitize unbroken skin. Additionally, they’re highly effective for cleaning medical devices before application.
Alcohol-free prep wipes, in comparison, are gentle, non-irritating, and don’t sting fragile or broken skin. They often form a protective barrier on the skin, enhancing the adhesion of dressings and improving patient comfort. Many doctors will use alcohol-free skin-prep wipes to minimize pain, reduce irritation, and sterilize periwound skin.
Specialized Preps for Fragile or Pediatric Skin
Many skin-prep products prioritize no-sting, alcohol-free formulas for fragile, elderly, or pediatric skin. One of the most respected examples is Smith & Nephew’s NO-STING SKIN-PREP wipes and sprays, mentioned earlier.
They are pediatric tested, provide up to 96 hours of protection, and are both non-toxic and hypoallergenic. With a water-based polymer solution and a transparent barrier, it’s suitable for children as young as 1 month old.
When to Seek Professional Care
Managing a wound at home can often be complex, confusing, and difficult. This is particularly true when you’re unsure whether the wound is infected or is healing slowly. Consider seeking professional care if you’re dealing with:
Increased warmth, redness, or swelling
Foul odor
Unusual drainage of any kind
Fever or chills
Red streak extending from the wound
A wound that isn’t healing after 10 days
Wounds exceeding ¾ inch long or ½ inch deep
Animal bites or human bites
Punctures from rusty or dirty objects
A wound care specialist can effectively diagnose and treat these conditions, with proven outcomes and measurable impact. Waiting is not worth the risk of reducing your quality of life—or increasing your risk of chronic wounds.
Related: When to See a Wound Care Specialist: Signs It’s Time to Get Expert Help

Integrating Skin Prep Into Home Wound Care Routines
Keep supplies organized.
When managing a wound at home, keep all supplies organized and sanitary. This reduces confusion and minimizes the risk of applying unnecessary products, dressings, or treatments. Additionally, it ensures every supply necessary for wound healing is free of contaminants or bacteria.
Follow a consistent dressing change schedule.
Routine care is essential in reducing irritation and improving outcomes. Consult with a wound care specialist to learn more about dressing schedules based on your unique situation. Remember: keeping dressing on for too long can delay healing, promote bacterial growth, and cause tissue damage.
Prioritize skin protection during adhesive removal.
While seemingly unlikely, skin tears and adhesive trauma (MARSI) are incredibly common when changing dressings or medical devices. It’s increasingly common among elderly, fragile, or sensitive skin. Prioritizing skin prep, however, can significantly reduce additional damage by making removal both gentler and safer.
Monitor the periwound skin at every change.
When changing dressings, tape, and medical devices, continuously monitor the periwound skin. Doing so reduces the risk of wound enlargement, maceration, inflammation, or contact dermatitis. If these symptoms are present, early detection is crucial for proper treatment and infection prevention.
Skin prep for wound care is essential for faster healing, improved outcomes, and protecting the periwound environment throughout treatment.
Wound healing often seems like a complex, dynamic process. While different injuries require different procedures, one thing remains true: skin prep is key in facilitating safe, effective recovery. With proper techniques and evidence-based guidance, healing becomes more manageable, comfortable, and successful—both in clinical and home-care settings.
At Royal Wound Care, our team specializes in comprehensive, advanced wound treatment. With a commitment to improving care and making treatment more accessible, every patient can expect to receive the attention and expertise they deserve.
For SNFs and independent nurses, we encourage you to review our educational opportunities and professional partnerships. When partnering with Royal Wound Care, you can expect faster healing times, lower infection rates, and fewer wound-related hospitalizations. The future of patient satisfaction and quality of life begins here!
Request an Appointment at a Royal Wound Care Facility near you.
Royal Wound Care is the expert in wound healing. Our board-certified wound care specialists are ready to help you begin your healing journey. Click the button below to request an appointment at a Wound Care Center near you—no referral needed
© 2025 Royal Wound Care, LLC. All rights reserved.
site by Growth Partners Marketing
