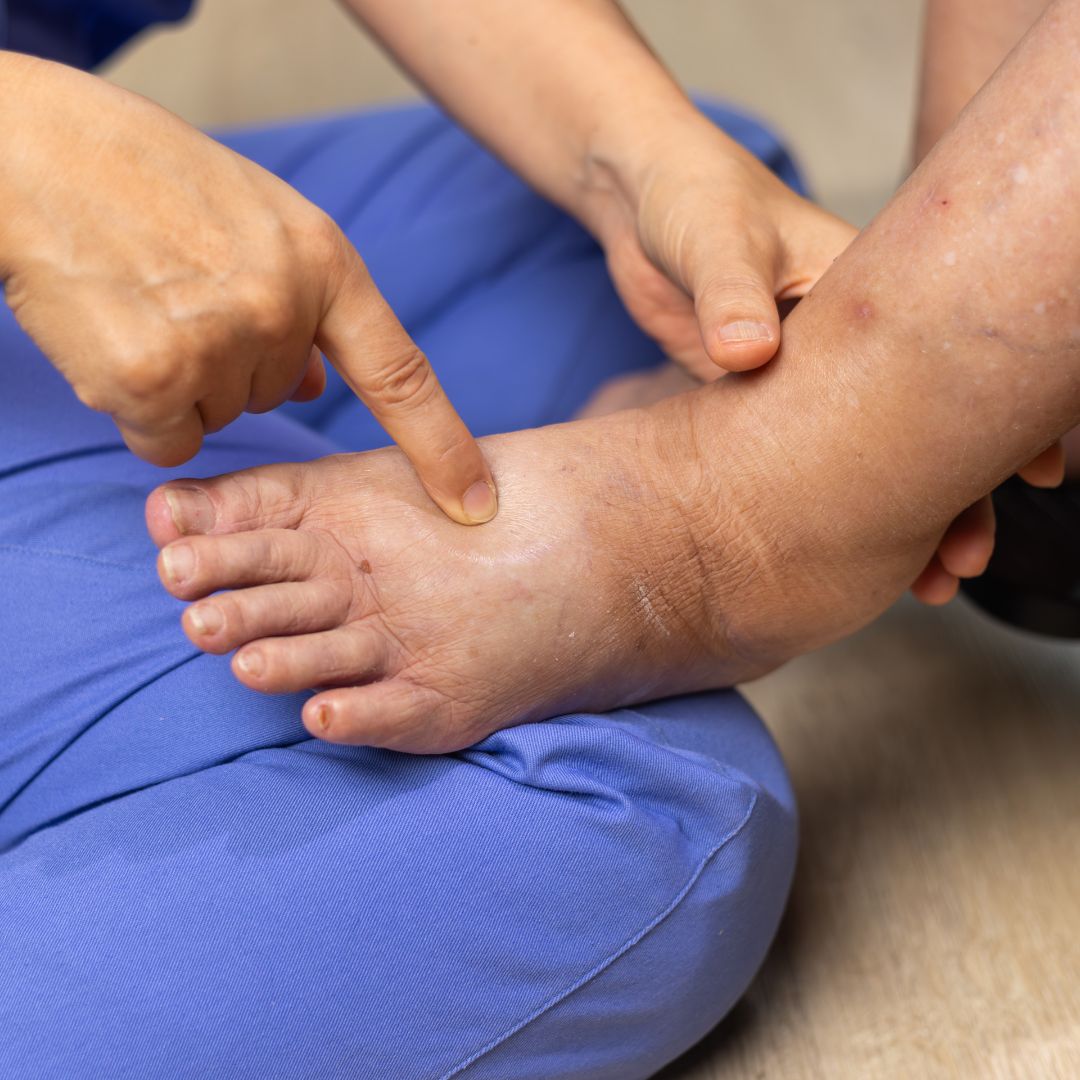
Diabetic Foot Ulcer Treatment in West Hills, California
Diabetic Foot Ulcer Treatment in West Hills, California
Diabetic foot ulcers (DFUs) are one of the most common—and most serious—complications of diabetes. Affecting approximately 15% of people with diabetes, DFUs can begin subtly, often as a blister or sore spot, and quickly progress without proper care. If not treated early, patients can experience infections, long-term tissue damage, and, in severe cases, extremity amputation.
What makes diabetic foot ulcers especially concerning is how easily they go unnoticed. Nerve damage and poor circulation result in a loss of sensation, preventing patients from experiencing pain until the condition has progressed. This is why understanding the warning signs and seeking timely professional wound care is critical.
For those in West Hills, California, board-certified clinics like Royal Wound Care prioritize early intervention, advanced treatment methods, and patient education. Through compassionate, expert-level care, you can get ahead of progressive symptoms and reduce the risk of serious complications before they impact your long-term health.
Below, we will discuss what you need to know about diabetic foot ulcer treatment in West Hills. We will discuss what DFUs are, what causes them, how to effectively treat them, and where to find professional help. With this information, you can better understand warning signs—and most importantly, your treatment options.

Diabetic Foot Ulcer Treatment in West Hills, California
Diabetic foot ulcers often advance rapidly, especially without proper care. The combination of peripheral neuropathy (nerve damage), poor circulation, and immune dysfunction impairs healing, turning superficial injuries into deep-tissue infections.
However, while this seems intimidating, early diagnosis and professional treatment can significantly improve outcomes. More specifically, when taking a proactive approach and seeking board-certified care, the risk of complications is considerably reduced.
To learn more, visit our guide, “Diabetic Wounds on Legs,” next. For now, we will discuss what a diabetic foot ulcer is and why you may be experiencing one.
What Is a Diabetic Ulcer on the Foot?
A diabetic foot ulcer is an open sore or wound that develops on the bottom of the foot, particularly at pressure points such as the ball or heel. Generally, DFUs occur due to a combination of diabetic neuropathy (nerve damage), peripheral artery disease (PAD), repetitive pressure, and immune system dysfunction.
Individuals with diabetes are often at higher risk for complications, especially when managing unstable blood sugar levels. With a loss of sensation, many patients are unaware of damage that may quickly worsen. Paired with poor circulation and a lack of blood flow, diabetic foot ulcers can develop rapidly, become infected, and lead to serious complications.
According to research, approximately 50,000 amputations in the United States are due to DFUs. Moreover, the American Diabetes Association claims limb amputations due to diabetes occur every 3 minutes and 30 seconds.
This is why at Royal Wound Care, we prioritize ongoing education, expert-led care, board-certified providers, and advanced modalities. We aren’t just here for the initial diagnosis—we stand by patients through every stage of healing. For patients in West Hills, we will provide directions to our office below.
For those outside of California, we encourage you to continue reading for guidance on recognizing symptoms, understanding treatment options, and knowing when to seek specialized care.
Here is how to reach the Royal Wound Care office in West Hills.

What Causes Diabetic Ulcer in the Foot?
Peripheral Neuropathy
Peripheral neuropathy is damage to nerves that results in numbness, tingling, burning, and weakness. There are two different types of neuropathy, including:
Sensory Neuropathy: Nerves cannot detect pain or temperature changes, resulting in a lack of sensation and paresthesia
Motor Neuropathy: Damage to nerves that control muscles can lead to deformities, creating additional pressure points on the foot
Individuals with diabetes often experience both, which is referred to as diabetic sensorimotor polyneuropathy (DSPN). In these cases, patients place pressure on abnormal areas of the foot as they continue walking barefoot or wearing tight shoes. Because they may not feel wounds as they develop, they unintentionally overlook early signs of injury or infection.
Related: Wound Dressing for Pressure Ulcers
Poor Blood Circulation
Poor blood circulation is a condition in which blood flow to the extremities becomes restricted, limiting the delivery of oxygen and nutrients. For people with diabetes, poor circulation is often a result of Peripheral Artery Disease (PAD), a circulatory condition that narrows the arteries and reduces blood flow to the legs and feet.
Whenever you experience a wound, the body delivers oxygen and nutrients to the area to fuel the repair process. For foot ulcers in patients with diabetes, inadequate blood flow can significantly impair healing. If the ulcer area cannot repair itself, it can result in tissue necrosis, breakdown, toxic buildup, and continued trauma.
Repeated Pressure or Friction
Both repeated pressure and friction play a significant role in the development of diabetic foot ulcers. Areas of the foot that withstand constant pressure, such as the heels, balls of the feet, and toes, are more vulnerable to skin breakdown. Individuals with total sensation are able to recognize discomfort and make immediate changes to reduce pain.
People with diabetes, because they often lack sensation due to neuropathy, remain aware of consistent pressure or friction. Over time, this can result in blisters, skin breaks, or minor tears. However, when combined with a lack of blood flow, the area cannot heal effectively. This is one reason why many minor blisters turn into chronic wounds and worsening ulcers.
Poorly Fitting Shoes
Wearing shoes that are too tight, too loose, or lack support can increase the risk of friction, create pressure points, and lead to skin breakdown. As mentioned previously, individuals with diabetes, especially those with reduced sensation, may not notice this quickly enough.
By the time they remove their shoes and socks, a wound may already have formed—or be worsening. Prompt attention can reduce the likelihood of complications and infections. However, without specialized care, this significantly increases the risk of ulcer formation.
High Blood Sugar Levels
Consistently elevated blood sugar levels (hyperglycemia) can interfere with the body’s natural healing process and weaken the immune system. Over time, these factors can contribute to nerve damage and poor circulation, both of which directly increase the risk of DFU development. This creates an environment where ulcers heal more slowly, infections are more likely, and the risk of complications increases.
What Does a Diabetic Foot Ulcer Look Like?
The appearance of a diabetic foot ulcer naturally progresses over time. In the early stages, it often appears as a small, shallow red crater or blister with thick, callused skin surrounding it. In addition to appearance, the wound may either bleed or drain serous fluid.
As it progresses, the ulcer develops into a wider, deeper, open crater-like wound surrounded by calloused skin. It can appear red if it's inflamed or yellow, brown, or black if it contains necrotic tissue. Moreover, you may notice a foul odor, swelling, or increased warmth that spreads away from the wound.
To better understand what stage your diabetic foot ulcer is in, here is a brief breakdown:
Stage 0–1: Skin is warm, red, and slightly swollen. It will first appear as a callous or blister, with a light pink or red crater.
Stage 2: The ulcer begins to deepen, extends into the soft tissue, and appears as a deeper, redder crater.
Stage 3: The base of the wound may appear yellow or black, indicating necrotic (dead) tissue.
Stage 4–5: The wound begins to look gangrenous, indicating an infection may be spreading to the bone or deeper tissues.
Understanding the signs, stages, and appearances of diabetic foot ulcers can help you make more informed care decisions. More importantly, it can help you communicate your symptoms and experiences with your wound care specialist.
Related: How Can a Diabetic Wound Heal Faster?
How do Diabetic Foot Ulcers Start?
Most diabetic foot ulcers begin as minor injuries, such as cuts, blisters, or abrasions. When caught early, you can speed the healing process up and reduce the risk of further complications. However, when experiencing reduced sensation and blood flow, people with diabetes often don’t realize a wound has developed to begin with.
Without prompt attention and proper care, the wound inevitably worsens over time. This is especially true if the patient continues walking barefoot, wearing poorly fitting shoes, or creating friction against the ulcer area.
Additionally, poor circulation plays a significant role in wound progression. Because the area is not receiving adequate nutrients and oxygen, it’s hard for the tissue to repair itself as efficiently as it would otherwise. This is why it’s important to cleanse the wound daily, apply a wound dressing or bandage, and monitor any changes.
Most importantly, however, is understanding your care options and reaching out to a board-certified wound care specialist. Below, we will discuss how your provider will treat a diabetic foot ulcer, whether through in-clinic wound care at our West Hills office or mobile wound care for better accessibility.

How to Treat Diabetic Foot Ulcer
Cleaning and Dressing the Wound
When managing a diabetic foot ulcer, proper hygiene is essential. Wound care specialists commonly cleanse the ulcer in patients with diabetes using sterile saline solution or non-cytotoxic wound cleansers. Most importantly, many specialists ensure they avoid harsh antiseptics, such as alcohol, iodine, or hydrogen peroxide, as they can damage fibroblasts and slow healing.
Removing Dead Tissue
Debridement, a process of removing damaged, infected, or necrotic tissue, is standard across wound care specialty clinics. Ultimately, this skin can harbor significant bacteria that may spread rapidly to healthy tissue, resulting in severe complications. By reducing bacterial load and clearing the wound bed, debridement promotes healing and supports advanced treatments.
Reducing Pressure
A significant amount of DFUs are caused by excessive pressure, making offloading an essential step in treatment. Wound specialists will often remove pressure by encouraging patients to shift their weight to unaffected areas, wear special, removable boots, or apply padding to the foot to create a cushion. By redistributing pressure, this approach helps prevent further tissue damage and promotes healing.
Managing Infection with Medication
If a patient’s diabetic foot ulcer is also infected, specialists will prescribe targeted antibiotic therapy to encourage growth factor production and prevent complications. Mild infections, for example, can often be treated with oral antibiotics. However, more severe cases require either stronger antibiotics or, in some cases, parenteral IV antibiotics.
Controlling Blood Sugar Levels
Maintaining stable blood sugar levels is critical to encouraging optimal healing of diabetic foot ulcers. When blood sugar remains elevated, healing slows, nerve damage progresses, and circulation remains impaired. Ultimately, these factors, especially in combination, slow healing and increase the likelihood of complications.
What Is the Best Treatment for Diabetic Foot Ulcer in West Hills? Choosing Royal Wound Care
Located in and serving West Hills and the greater San Fernando Valley, Royal Wound Care provides comprehensive, evidence-based care for diabetic wounds. Patients can expect personalized treatment plans, advanced therapies, and a strong emphasis on education to prevent recurrence.
At a board-certified clinic like Royal Wound Care, treatment goes beyond basic management. We stand with patients from diagnosis to resolution, offering the highest level of wound management and evidence-based solutions. Through cutting-edge research and a highly trained, board-certified staff, you can receive the quality, attentive care you deserve.
For questions, call the Royal Wound Care team today. We honor the ability to walk you through every step of the process—providing expert guidance, personalized care, and the support you need to heal with confidence. And for individuals located in West Hills, Woodland Hills, Canoga Park, Calabasas, Chatsworth, or the San Fernando Valley, visit our website to schedule an appointment.
At Royal Wound Care, we aren’t just specialists—we’re compassionate advocates who prioritize your healing, guide you through every stage of care, and ensure you feel supported, informed, and confident throughout the process.
Related: What Does It Mean to be Board-Certified in Wound Care?
Frequently Asked Questions About Diabetic Foot Ulcer
What percentage of patients with diabetes develop foot ulcers?
Approximately 15–25% of patients with diabetes may develop a diabetic foot ulcer at some point. Moreover, this condition remains the most frequent reason people with diabetes are hospitalized. It’s important to inspect your feet daily, wear special footwear, reduce the amount of time you walk barefoot, and manage blood sugar levels. If you begin to notice swelling, cuts, or blisters, do not be afraid to reach out for help.
Are diabetic foot ulcers painful?
Not always. In fact, many patients do not experience pain due to a loss of sensation in the feet (peripheral neuropathy). Even in advanced cases, it’s not uncommon for patients to feel little to no pain. In most cases, you may only begin to feel pain in the presence of an infection, which can cause swelling, burning, or stinging in surrounding areas.
Do diabetic foot ulcers itch?
Yes, diabetic foot ulcers can definitely cause the surrounding skin to itch. This is often the result of dry skin and poor circulation. Moreover, because many DFUs are prone to infections, the infection itself can cause itchiness until it’s properly healed. Nonetheless, it’s essential to keep the ulcer clean and bandaged to reduce the risk of reinjury.
If you’re dealing with a diabetic foot ulcer in West Hills, visit Royal Wound Care today.
Diabetic foot ulcers can progress quickly, which makes treatment feel intimidating. However, with early intervention and expert care, they are highly manageable. If you notice any changes in your feet, even something minor, it’s always best to seek advice from a board-certified wound care specialist. Timing makes all the difference.
Alongside quality, board-certified care, we also feature educational resources and partnership opportunities to both SNFs and independent nurses. With proper leadership, we support improved healing outcomes, reduce infection risk, and minimize wound-related hospitalizations—one patient at a time.
